How to Tell the Difference Between Nummular Eczema and Ringworm
It’s often difficult to distinguish between nummular eczema and ringworm, so it’s always best to be evaluated by a dermatologist, say experts.
Published On: Feb 20, 2017
Last Updated On: Jan 23, 2023
Contact Dermatitis (CD) is a term used to describe the itchy skin reaction that can occur following topical contact (and sometimes oral, or airborne) with allergy-producing chemicals in the environment.
Our skin serves as a protective barrier. When that protective barrier is disrupted, foreign substances can penetrate the skin and prompt the immune skin cells to take action. In doing so, these immune cells create inflammation in which various protective substances get released into the blood stream and onto the skin to fight off the foreign substance. Unfortunately, there can be damage to the skin during this battle. Thus, although our body’s response was intended to be protective, it actually participates in the skin damage.
There are many types of contact dermatitis. That being said, the three most frequent types are irritant, allergic, and contact urticaria (hives).
Irritant contact dermatitis (ICD) is the most common type of contact reaction. It can develop at the first sign of contact between our skin and an abrasive or irritating chemical (i.e. soap), physical interaction (i.e. friction), or biologic substance (i.e. heat). These substances are able to break through the barrier and stimulate skin inflammation.Of note, if the skin is already compromised with a wound, or a chronic skin-barrier disease such as atopic dermatitis (AD), it is much easier for these substances to enter and, thus, the risk for developing irritant contact dermatitis is much higher.
Allergic contact dermatitis (ACD) is the second most common reaction type and is delayed in its nature. In order for a reaction to occur, the immune system must first be able to recognize the foreign substance.
The first time the skin comes in contact with a new allergen, it sends a piece (hapten) of it off to the immune system for analysis, and storage in the immune system’s memory bank. This process is called sensitization. At the first meeting between the skin and the allergen there is no skin reaction.
When the skin comes into contact with the substance again and again, the immune system remembers it and develops an itchy skin response. Because it can take a few days for the immune system to go through the memory bank and recognize the chemical, the skin reaction may be delayed for 48 to 96 hours after the actual exposure.
Contact urticaria (CU) is a less common form of contact dermatitis and is characterized by a wheal and flare reaction (aka hives), local swelling and redness that can occur immediately after skin contact with an offending substance, but is usually not long-lasting. Contact urticaria is distinguished by the rare but serious risk of an anaphylactic reaction that can coincide with the skin inflammation.Although we note the importance of contact urticaria, this article will focus on the two main types ACD and ICD.
Irritant contact dermatitis can develop from chemical or physical contact with an irritating substance on the skin surface. The irritants cause damage to the skin barrier, which then results in an impaired skin barrier and red itchy skin rashes.
In allergic contact dermatitis, the allergens may come into direct contact with the skin through household products or personal care products, may be airborne or may come from an ingested source. Other times, a skin reaction can occur from contact with an individual (a partner or close-contact) who utilized a chemical their child or spouse is allergic to, such as fragrance or hair dye.
There are many different triggers for contact dermatitis.
ICD may develop from everyday substances such as water, mechanical factors such as pressure or friction, and environmental changes such as extremes of temperature and humidity.
There are a large number of potential allergy-producing chemicals. Here we present the common ones that are problems for patients with atopic dermatitis:
Nickel allergy is extremely common among adults and children. Nickel is found in a range of metallic items, such as jewelry, zippers, buttons, belt buckles, and coins. Also, patients become exposed from some less obvious sources such as cell phones, white gold, certain orthopedic joint replacements, and certain foods (even chocolate!).
Cobalt is a common contaminant in various metals, including nickel, and patients allergic to nickel are often inherently allergic to cobalt because of its widespread use. Patients who are allergic to one metal may also “co-react” to another due to common source exposures and co-sensitization.
Chromium salts, often found in paints, cement, and leather products may induce ACD and sometimes irritant contact dermatitis.
Fragrances are also common culprits of allergic contact dermatitis especially in persons with disrupted skin barriers, such as atopic dermatitis. These substances can be found in various cosmetics, perfumes, food flavorings, and toothpastes.
Antibacterial ointments such as neomycin and bacitracin are often used to treat everyday scratches and wounds, but some people develop allergic reactions to these.
Formaldehyde a commonly known as a preservative favored for its disinfectant properties, but it is also a top adult and child allergen. It is a ubiquitous chemical found in many different products including household disinfectants and vaccines, glues and adhesives, cigarette smoke, and embalming fluid. Notably, formaldehyde-releasing preservatives are utilized in personal care products and may trigger some individuals who are allergic to formaldehyde. Further hidden sources include “permanent press” and “wrinkle- resistant” clothing, and aspartame!
Isothiazolinones, including methylchloroisothiazolinone and methylisothiazolinone (MCI/MI),are another type of preservative used in many personal care products to inhibit fungi and bacterial growth, as well as to protect the product from oxygen and light as these can lead to damage or degradation.
It is often found in many “wash-off” items such as shampoos, body washes, and cosmetics. Importantly, recent reports have found this ingredient in wet wipes, baby wipes, and moistened toilet tissues.
Cocamidopropyl betaine (CAPB) is a detergent chemical used to thicken shampoos, soaps and lotions, and reduce static cling in clothing. Clothing and skin care products containing this chemical may be irritating to individuals with AD and should definitely be avoided in those with known sensitivity.
Paraphenylene-diamine (PPD) is a strong sensitizing chemical that is used in hair-dye. It is prohibited in skin-contacting products due to the allergy potential. Nevertheless, PPD continues to be used in various unregulated products such as black hen temporary tattoos, which are frequently found in child-friendly environments such as vacation destinations, county fairs, and beach resorts. PPD is often used to dye shoes black, and can cross-react with dyes used in clothing and some medications, such as antihistamines!
These terms are often used by manufacturers to imply a lower risk of developing an allergic reaction to their product, however, the use of these slogans is not regulated. This means that the ingredients may still contain known allergens! If a product contains an ingredient that a patient is allergic to, they should avoid it. Always read the label!
Irritant contact dermatitis is usually confined to the location where exposure occurred. If the exposure is to a strong irritant, an immediate reaction including pain, swelling, and even blistering can be present. If there is chronic exposure to a mild irritant such as water or soap, the reaction can occur over a period of weeks to months and involve dryness, itching, and cracking—this is often seen on the hands.
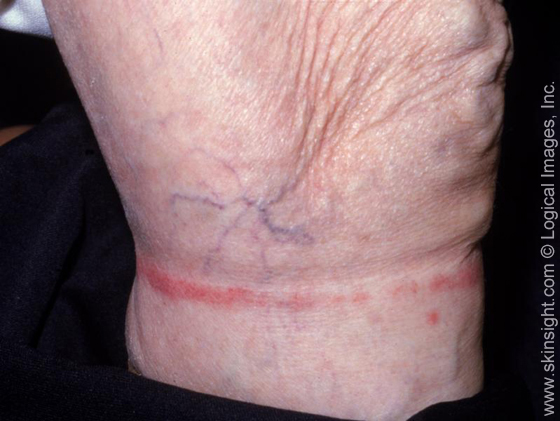
Allergic contact dermatitis may also be limited to the site of original contact, but more often spreads beyond the site of contact. The skin becomes red, hot, itchy and may weep. Classic examples are earlobes reacting to costume jewelry, belly reactions to belt-buckles containing nickel, and poison ivy reactions.
Contact dermatitis can sometimes be very difficult to distinguish from atopic dermatitis. Consulting with a dermatologist is key for correct diagnosing.
Patch testing is an important tool in the diagnosis of allergic contact dermatitis. To perform this diagnostic test, selected chemicals are prepared in disks on an adhesive strip and applied to the patient’s back, where there is no rash.
The patches are left on for 48 hours during which time the patient is advised not to shower, so as not to alter the results.
On the first follow-up visit the provider removes the patches and evaluates the skin for reactions. The patch application sites are then reexamined after two more days to look for signs of inflammation.
If there is inflammation in a specific location where an allergen was placed, the allergy is confirmed and the provider can inform the patient how to avoid that allergen to prevent recurring rash.
If you experience unusual skin redness and itching, you may want to seek medical advice from a health care provider, as they can help determine the cause of the reaction and recommend treatment options.
The best treatment for contact dermatitis is avoidance. Providers have access to narratives and lists of products where these allergy chemicals are found, and they are available for free for patients—please see the resources guide at the end of this article.
In addition, some providers who often treat contact dermatitis subscribe to electronic programs that will create shopping lists free of allergens for patients, such as the Contact Allergen Management Program (CAMP), and the Contact Allergen Replacement Database (CARD).
Additionally, your health care provider may prescribe a topical or oral medication to treat your rash, in addition to avoidance.
American Contact Dermatitis Society
Contact Allergen Management Program (CAMP)
Contact Allergen Replacement Database (CARD)
Contact Dermatitis Resource Center
 Alina Goldenberg is a University of California, San Diego School of Medicine fourth-year medical student, and a Master’s in Clinical Research candidate.
Alina Goldenberg is a University of California, San Diego School of Medicine fourth-year medical student, and a Master’s in Clinical Research candidate.
 Sharon E. Jacob, MD, is an Associate Professor and Director of the Contact Dermatitis Clinic at Loma Linda University in the Department of Dermatology. She has served as an independent investigator on the safety and efficacy of T.R.U.E. Test™ (Smart Practice; Phoenix, AZ) panels 1.1, 2.1, and 3.1 in children and adolescents, Pediatric Research Equity Act (PREA-1) trial, and now serves as an investigator on PREA-2.
Sharon E. Jacob, MD, is an Associate Professor and Director of the Contact Dermatitis Clinic at Loma Linda University in the Department of Dermatology. She has served as an independent investigator on the safety and efficacy of T.R.U.E. Test™ (Smart Practice; Phoenix, AZ) panels 1.1, 2.1, and 3.1 in children and adolescents, Pediatric Research Equity Act (PREA-1) trial, and now serves as an investigator on PREA-2.