Atopic Dermatitis
What is atopic dermatitis?
Atopic dermatitis (AD) is the most common type of eczema, affecting more than 9.6 million children and about 16.5 million adults in the United States. It’s a chronic condition that can come and go for years or throughout life, and can overlap with other types of eczema.
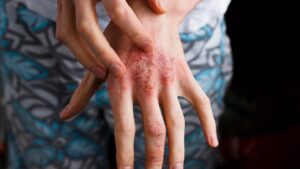
In people with AD, for complex reasons science hasn’t fully sorted out, the immune system becomes disordered and overactive. This triggers inflammation that damages the skin barrier, leaving it dry and prone to itching and rashes that may appear purple, brown or grayish hue in darker skin tones and red in lighter skin tones.
Research shows that some people with eczema, especially atopic dermatitis, have a mutation of the gene responsible for creating filaggrin. Filaggrin is a protein that helps our bodies maintain a healthy, protective barrier on the very top layer of the skin. Without enough filaggrin to build a strong skin barrier, moisture can escape and bacteria, viruses and more can enter. This is why many people with AD have very dry and infection-prone skin.
Who gets AD and why?
Atopic dermatitis typically begins in childhood, usually in the first six months of a baby’s life. Even though it’s a common form of eczema, it’s also severe and long-lasting. When you or your child have atopic dermatitis, it may improve at times; but at other times, it may get worse. In some children, symptoms may taper off as they grow up, while other children will have atopic dermatitis flares into adulthood.
Atopic dermatitis exists with two other allergic conditions: asthma and hay fever (allergic rhinitis). People who have asthma and/or hay fever or who have family members who do, are more likely to develop AD.
What are the symptoms of AD?
Itching is the hallmark of AD, with some data showing that more than 85% of people with the condition experience this distressing symptom every day. Sore or painful skin and poor sleep caused by itching are also common.
People with AD can get rashes anywhere on the body that can ooze, weep fluid and bleed when scratched, making skin vulnerable to infection. Skin can become dry and discolored, and repeated scratching can cause thickening and hardening — a process called lichenification.
How is AD treated?
When AD is mild, management may include:
- avoiding known triggers
- maintaining a regular bathing and moisturizing routine to protect and strengthen the skin barrier
- getting high-quality sleep
- eating a healthy diet
- managing stress
If these methods are not enough, other treatments include:
- topical corticosteroids
- non-steroidal topicals
- biologics
Read more about eczema treatments.
What do the ecz-perts have to say?
With atopic dermatitis, there is often “a vicious cycle of itching, scratching and more itching that further inflames the immune system and further damages the skin barrier,” said Dr. Peter Lio, clinical assistant professor of dermatology and pediatrics at Northwestern University’s Feinberg School of Medicine.
“AD is not just a ‘skin rash,’” Lio said. “It can have a huge impact on quality of life — not just that of the patient, but on family and friends too. The itch can make it difficult to concentrate, poor sleep can make people feel like zombies during the day, and treatments and precautions can take a toll on time, energy and money.”
“While there is no cure — yet — and AD can be difficult to treat, our understanding of it continues to improve and there is great hope and some amazing new treatments and approaches,” Lio said.