How to Tell the Difference Between Nummular Eczema and Ringworm
It’s often difficult to distinguish between nummular eczema and ringworm, so it’s always best to be evaluated by a dermatologist, say experts.
Published On: Sep 24, 2022
Last Updated On: Sep 30, 2023
There are more than 31 million Americans with eczema, and yet no two patients experience the condition the exact same way. How is this possible? We know there are seven different types of eczema, but what makes each of them unique? We spoke with Dr. Peter Lio, assistant professor of dermatology and pediatrics at Northwestern University, and Dr. Jeff Yu, an expert in contact dermatitis at Massachusetts General Hospital, to get the details on the underlying similarities and differences between the seven different types of eczema.
The short answer is yes: classifying different subtypes of eczema DOES help with diagnosis and treatment. They are all different in their own ways and have a varied combination of symptoms, triggers and genetic components. Dr. Lio suggested that healthcare providers might “actually need even more differentiation, ideally getting classification down to the molecular level.” He explained that healthcare providers “want to fully understand a patient’s condition in order to find the best, most targeted therapy to get things back in balance. Knowing the subtype of eczema helps doctors know what to look for, how to give patients counseling about the prognosis and triggers for the disease and it informs treatment options greatly.”
Atopic dermatitis (AD) is the most common type of eczema, affecting more than 9.6 million children and 16.5 million adults in the United States. For complex reasons that researchers are still studying, the immune system becomes overactive, triggering inflammation that damages the skin barrier, leaving it dry and prone to itching, rashes and infection.
AD is usually treated with moisturizing lotions, topic corticosteroids, non-steroidal topicals and biologics. Lifestyle changes to lower stress and ensure regular sleep and healthy dietary habits can also help.
How to know if you have it: AD can appear anywhere on the body and at any time of life, but it often appears in childhood and tends to be chronic. It can be hereditary and it is more likely to happen to people who have asthma, hay fever and/or food allergy.
Contact dermatitis occurs when your skin becomes irritated or inflamed in response to physical contact with an allergen; unlike atopic dermatitis, contact dermatitis does not run in families and isn’t associated with other allergic conditions such as asthma or allergic rhinitis. Standard treatments include topical steroids, as well as patch testing to determine the source of the allergen.
How to know if you have it: Contact dermatitis can appear out of the blue and typically disappears when the allergen or irritant is removed. It usually occurs in the spot where your body comes into contact with the allergen or irritant.
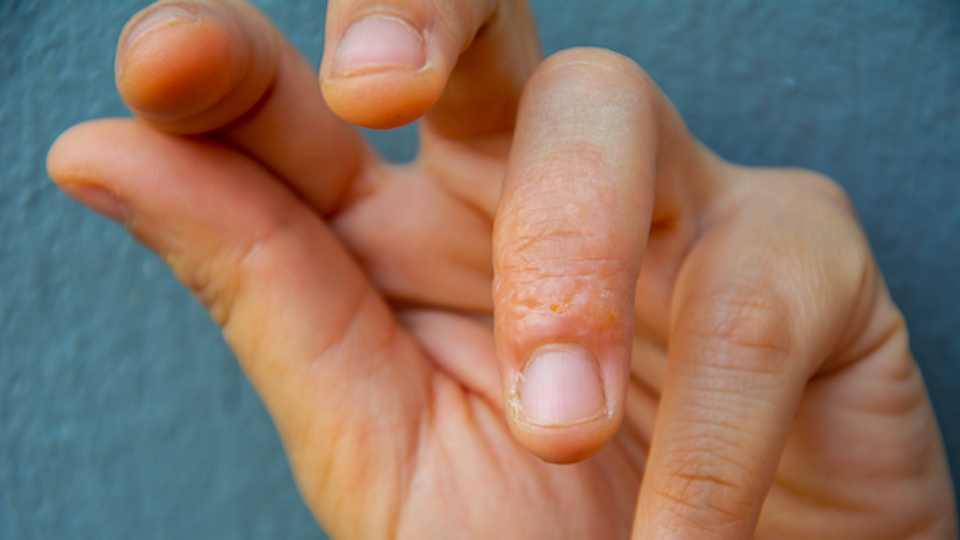
Dyshidrotic eczema, alternatively called pompholyx, causes small, itchy blisters on your toes, soles of your feet, palms of your hands and fingers. While the cause is unknown, this type of eczema does tend to run in families. In addition to recommending a rigorous skincare regimen with moisturizers, dyshidrotic eczema is also treated with light therapy, topical calcineurin inhibitors or oral steroids.
How to know if you have it: Dyshidrotic eczema usually only occurs on the hands and feet. It’s characterized by small, intensely itchy blisters.
Neurodermatitis, also known as lichen simplex chronicus, is a common type of eczema that starts with an itchy patch of skin. Scratching that patch causes more intense itching and then, over time, chronic scratching causes the itchy patches of skin to become dry, leathery and thickened. Neurodermatitis can be triggered by stress, tight clothing (particularly when made from wool or synthetic fabric), bug bites, nerve injury and dry skin.
Unlike atopic dermatitis, which can be widespread, neurodermitis is usually confined to one or two patches of skin. It rarely goes away without treatment and continued scratching can irritate nerve endings in skin, intensifying both itching and scratching.
Treatment for neurodermatitis is aimed at healing skin and ending the itch-scratch cycle. Treatments can include topical corticosteroids, calcineurin inhibitors and ointments made with salicylic acid to control the itch. Occlusive therapies to block scratching and behavioral therapies are also used.
How to know if you have it: Neurodermatitis is usually confined to one or two patches of skin in areas where you can reach to scratch. It’s characterized by thick, scaly patches of skin. Neurodermatitis is most common in adults between 30 and 50 years of age and occurs most often in women and in people with contact dermatitis and atopic dermatitis.
Nummular eczema, also referred to as discoid eczema and nummular dermatitis, features scattered circular, often itchy and sometimes oozing patches. This form of eczema can develop due to dry skin, skin trauma or as a reaction to allergens or irritants.
Nummular eczema can look like psoriasis, ringworm, fungal infection and other types of eczema, including atopic dermatitis, stasis dermatitis and contact dermatitis. Once correctly diagnosed, it tends to disappear completely with the right treatment, which can include mid- or high-potency topical corticosteroid, along with a topical antibiotic. If eczema patches are substantially weepy and oozy, application of an astringent compress can help dry the area and drive out any staph infection.
How to know if you have it: Nummular eczema can be identified by its coin-shaped, itchy, oozing lesions that frequently appear on arms, legs, torso and hands.
Seborrheic dermatitis, also called “cradle cap” in infants, is an itchy, scaly rash that occurs in places on the body where there many oil-producing glands, such as the upper back, nose and scalp; the inflammation is caused by a reaction to excess Malassezia yeast that typically lives on the skin’s surface.
Mild cases are usually treated using a topical antifungal cream or medicated shampoo; if the condition is more severe, intermittent use of a topical corticosteroid or calcineurin inhibitor may be required.
How to know if you have it: Seborrheic dermatitis usually occurs on the upper back, nose, eyebrows and scalp and is recognizable by redness, swelling and greasy scaling. It’s more common in children and adults between 30 and 60 years old. Among adults and teens, it’s more common in men.
Stasis dermatitis, also called gravitational dermatitis, venous eczema, and venous stasis dermatitis, develops due to poor circulation in the legs. Stasis dermatitis symptoms include swelling of the feet, skin discoloration (brown, purple, grey or ashen in darker skin tones, and redness in lighter skin tones), itching, scaling and dryness.
Treatment for stasis dermatitis includes identifying and treating its root cause as well as controlling its various symptoms. Treatment to reduce swelling can include compression stockings, elevating legs, avoiding foods high in salt, topical steroids for inflammation and antibiotics if infection is present.
How to know if you have it: Stastis dermatitis typically appears in the feet and lower legs of people over 50 and who have poor circulation and occurs alongside other symptoms of poor ciruculation, like ankle swelling.
If you live with eczema, you probably know the answer to this one: they itch! All different types of eczema share the universal symptom of “pruritus,” or itchiness. But that’s not all. Dr. Lio explained that all seven types of eczema are also “type 2 (allergic type) inflammatory skin conditions that share some of the same signalling molecules (cytokines) such as IL-4, IL-13 and IL-31.” In other words, there is a biological commonality underlying all seven types of eczema. For more information about itch, check out our recent article “The Complex Science of Itch.”
According to Dr. Lio, soaps and detergents can trigger almost anyone to flare up in the right context. “I would also argue that stress is a fairly universal trigger,” he added. “Allergens are much more nuanced and individualized. Environmental stressors like heat and cold are fairly common, but not universal.”
If the itchiness is universal, and if soap and detergents can trigger any type of eczema, we asked Dr. Lio if there were any subcategories of eczema that stood apart from the rest. “The most different might be seborrheic dermatitis,” he said. “It is intimately connected to a yeast on the skin that does not seem to be playing the same role in other types of eczema.” He added that contact dermatitis is different, as well, because a patient may have “one key trigger for a flare and frequently when that flare is removed, the skin becomes 100% perfect and clear, unlike the other forms of eczema that have many potential triggers.”
For many patients, the challenging truth is that you can experience more than one type of eczema at the same time. Not only that, you can experience all of the different types of eczema, at different times, throughout the course of your lifetime. Dr. Lio explained that he frequently sees allergic contact dermatitis and atopic dermatitis in the same patient. “It’s very tough to separate them sometimes,” he said, “but that is why patch testing is so important.”
Knowing that each type of eczema has a unique profile, it’s especially important to connect with a dermatologist who can recognize and diagnose all seven types of eczema. Check out our summary of each type of eczema for more information about symptoms and triggers.