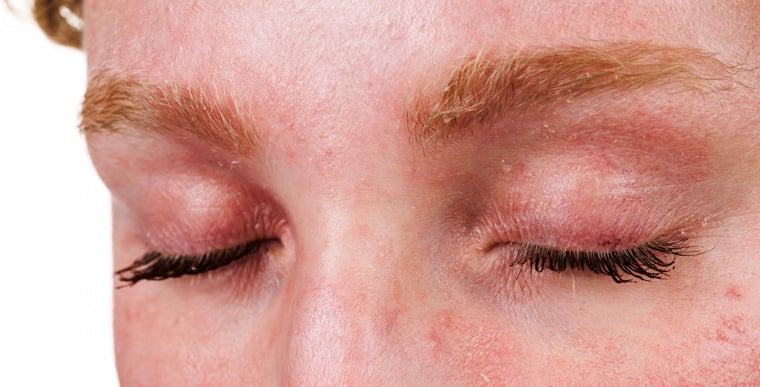
Eyelid eczema, also called eyelid contact dermatitis or periorbital dermatitis, is part of a group of inflammatory skin conditions that cause dry skin, itchiness, rashes, scaly patches, blisters and skin infections. It can appear in various places on the body, including the face, particularly the eyelids.
Eyelid eczema is quite common, affecting 15-20% of people at some point in their lives. The condition affects women more often than men, making up 73-80% of cases, largely due to greater use of cosmetic products. Allergic contact dermatitis is the single most common cause of eyelid eczema, accounting for 31-72% of cases, followed by atopic dermatitis at 14-39.5%.
Of the seven known types of eczema, a few can specifically impact the eyelids:
- Contact Dermatitis: Irritant contact dermatitis occurs when the skin is damaged by substances like skincare products, soaps or makeup, without involving an allergen. Allergic contact dermatitis, which is more common on the eyelids, happens when the skin reacts to allergens.
- Atopic Dermatitis: This form of eyelid eczema is caused by environmental or genetic factors and an overactive immune response that triggers inflammation, leaving skin dry, itchy and prone to rashes. Some people with this condition have a filaggrin gene mutation, which weakens the skin barrier and increases susceptibility to flare-ups.
- Seborrheic Dermatitis: This type affects oil-rich areas like the eyelids along the lash line, causing flaking, crusting or redness. Triggers may include cosmetics, environmental factors, genetics, stress, cold weather, hormonal changes and inflammatory reactions to Malassezia yeast on the skin.